Image

Barrier methods
Barrier contraception comes in several forms, like external and internal condoms, diaphragms and cervical caps. Read more about Barrier methodsImage

Emergency contraception
Emergency contraception can be used if contraception has not been used when having sex, or if the contraception used failed and pregnancy is unplanned. Read more about Emergency contraceptionImage
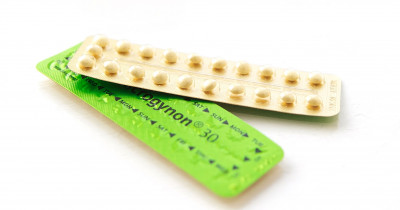
Hormonal contraception
There are many types of hormonal contraception: the pill, the mini pill, the contraceptive patch and the vaginal ring, as well as long-acting reversible contraception methods. Read more about Hormonal contraceptionImage


